Abstract
Purpose
The increased use of proton pump inhibitors (PPIs) in the elderly has raised concerns about potential severe adverse effects. Our systematic review investigated the mortality associated with PPI use in elderly populations.
Methods
We searched MEDLINE, EMBASE, and the Cochrane Library for relevant publications until August 2022. We included randomized controlled trials (RCTs), quasi-RCTs, and observational studies on the association between proton pump inhibitors and mortality in the elderly. To estimate the pooled relative risk (RR) and 95% confidence interval (CI), the inverse-variance random effect model was used. Heterogeneity was assessed using the I2 test. Subgroup analyses were performed by follow-up period, population, and study design.
Results
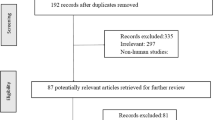
A total of 4 RCTs and 36 cohort studies were included in the meta-analysis. Four RCTs showed that there was no significant association between PPIs and the risk of death. From 23 observational studies (26 cohorts), the use of proton pump inhibitors was not significantly associated with increased mortality in the elderly (RR 1.14; 95% CI, 0.90–1.45). However, when controlling for covariates from 33 observational studies (41 cohorts), proton pump inhibitors in older adults aged 50 years or more were significantly associated with a 15% higher risk of mortality compared to nonusers (RR 1.15; 95% CI, 1.10–1.20).
Conclusions
Our meta-analysis of RCTs found that PPIs did not show a significant association with increased mortality risk in older adults. However, the meta-analysis of cohort studies and long-term follow-up studies showed a higher increased risk of death with PPI use in older adults. The prescription of PPIs in patients aged 50 years or older should be carefully considered.



Similar content being viewed by others
Data availability
The datasets generated during the current study are available from the corresponding author on reasonable request.
References
Franceschi M, Di Mario F, Leandro G, Maggi S, Pilotto A (2009) Acid related disorders in the elderly. Best Pract Res Clin Gastroenterol 23:839–848
Thomson AB, Sauve MD, Kassam N, Kamitakahara H (2010) Safety of the long-term use of proton pump inhibitors. World J Gastroenterol 16(19):2323–2330
Kantor ED, Rehm CD, Haas JS, Chan AT, Giovannucci EL (2015) Trends in prescription drug use among adults in the United States from 1999–2012. JAMA 314:1818–1831
AlMutairi H, O’Dwyer M, McCarron M, McCallion P, Henman MC (2018) The use of proton pump inhibitors among older adults with intellectual disability: a cross sectional observation study. Saudi Pharm J 26:1012–1021
Maes ML, Fixen DR, Linnebur SA (2017) Adverse effects of proton-pump inhibitor use in older adults: a review of the evidence. Ther Adv Drug Saf 8(9):273–297
American Geriatrics Society 2015 Beers Criteria Update Expert Panel (2015) American Geriatrics Society 2015 updated Beers Criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc 2227–2246
O’Mahony D, O'Sullivan D, Byrne S, O'Connor MN, Ryan C, Gallagher P (2015) STOPP/START criteria for potentially inappropriate prescribing in older people: version 2. Age Ageing 44:213–218
Brown JP, Tazare JR, Williamson E, Mansfield KE, Evans SJ, Tomlinson LA et al (2021) Proton pump inhibitors and risk of all-cause and cause-specific mortality: a cohort study. Br J Clin Pharmacol 87(8):1–12
Xie Y, Bowe B, Li T, Xian H, Yan Y, Al-Aly Z (2017) Risk of death among users of proton pump inhibitors: a longitudinal observational cohort study of United States veterans. BMJ Open 7(6):e015735
Xie Y, Bowe B, Yan Y, Xian H, Li T, Al-Aly Z (2019) Estimates of all-cause mortality and cause specific mortality associated with proton pump inhibitors among US veterans: cohort study. BMJ 365:l1580
Sharma M, Holmes HM, Mehta HB, Chen H, Aparasu RR, Sgug YCT et al (2019) The concomitant use of tyrosine kinase inhibitors and proton pump inhibitors: prevalence, predictors, and impact on survival and discontinuation of therapy in older adults with cancer. Cancer 125(7):1155–1162
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med 151(4):W65–W94
Higgins J, Thomas J, Chandler J, Cumpston M, Li T, Page M et al (2023) Cochrane handbook for systematic reviews of interventions: the Cochrane Collaboration, Version 6.3. Available from: https://training.cochrane.org/handbook. Assessed 1 Jan 2023
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Davies HT, Crombie IK, Tavakoli M (1998) When can odds ratios mislead? BMJ 316:989–991
Stare J, Maucort-Boulch D (2016) Odds ratio, hazard ratio and relative risk. Metod Zv 13:59–67
Zhang J, Yu KF (1998) What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA 280:1690–1691
Adelborg K, Sundbøll J, Schmidt M, Bøtker HE, Weiss NS, Pedersen L et al (2018) Use of histamine H2 receptor antagonists and outcomes in patients with heart failure: a nationwide population-based cohort study. Clin Epidemiol 10:521–530
Adelborg K, Sundbøll J, Schmidt M, Bøtker HE, Weiss NS, Pedersen L et al (2020) Use of acid-suppressant medications after diagnosis increases mortality in a subset of gastrointestinal cancer patients. Dig Dis Sci 65(9):2691–2699
Baek YH, Kang EJ, Hong S, Park S, Kim JH, Shin JY (2022) Survival outcomes of patients with nonsmall cell lung cancer concomitantly receiving proton pump inhibitors and immune checkpoint inhibitors. Int J Cancer 150(8):1291–1300
Baik SH, Fung KW, McDonald CJ (2022) The mortality risk of proton pump inhibitors in 1.9 million US seniors: an extended cox survival analysis. Clin Gastroenterol Hepatol 20(4):e671-681
Bakhshwin D, Alotaibi M, Ali AS, Althomali A, Alsuwat A, Alhamyani A et al (2022) Mortality predictors among COVID-19 elderly in Taif, Saudi Arabia. Infect Drug Resist 15:3213–3223
Bell JS, Strandberg TE, Teramura-Gronblad M, Laurila JV, Tilvis RS, Pitkälä KH (2010) Use of proton pump inhibitors and mortality among institutionalized older people. Arch Intern Med 170(17):1604–1605
Bradley ES, Howe E, Wu X, Haran JP (2019) Proton pump inhibitors and 180-day mortality in the elderly after Clostridium difficile treatment. Gut Pathog 11:29
Brozek W, Reichardt B, Zwerina J, Dimai HP, Klaushofer K, Zwettler E (2017) Use of proton pump inhibitors and mortality after hip fracture in a nationwide study. Osteoporos Int 28(5):1587–1595
Cetin H, Wurm R, Reichardt B, Tomschik M, Silvaieh S, Parvizi T et al (2020) Increased risk of death associated with the use of proton-pump inhibitors in patients with dementia and controls - a pharmacoepidemiological claims data analysis. Eur J Neurol 27(8):1422–1428
Cholin L, Ashour T, Mehdi A, Taliercio JJ, Daou R, Arrigain S et al (2021) Proton-pump inhibitor vs. H2-receptor blocker use and overall risk of CKD progression. BMC Nephrol 22(1):264
de Francisco ALM, Varas J, Ramos R, Merello JI, Canaud B, Stuard S, Optimizing Results in Dialysis (ORD) group et al (2017) Proton pump inhibitor usage and the risk of mortality in hemodialysis patients. Kidney Int Rep 3(2):374–384
Farhat N, Birkett N, Haddad N, Fortin Y, Momoli F, Wen SW et al (2020) Risk of adverse cardiovascular events following a myocardial infarction in patients receiving combined clopidogrel and proton pump inhibitor treatment: a nested case-control study. Drugs Real World Outcomes 7(3):191–203
Hálfdánarson ÓÖ, Pottegård A, Lund SH, Ogmundsdottir MH, Ogmundsdottir HM, Zoega H (2020) Use of proton pump inhibitors and mortality among Icelandic patients with prostate cancer. Basic Clin Pharmacol Toxicol 126(6):484–491
Hasselgren G, Lind T, Lundell L, Aadland E, Efskind P, Falk A et al (1997) Continuous intravenous infusion of omeprazole in elderly patients with peptic ulcer bleeding. Results of a placebo-controlled multicenter study. Scand J Gastroenterol 32(4):328–333
Jun T, Ozbek U, Dharmapuri S, Hardy-Abeloos C, Zhu H, Lin JY et al (2021) Antacid exposure and immunotherapy outcomes among patients with advanced hepatocellular carcinoma. Ther Adv Med Oncol 13:17588359211010936
Juurlink DN, Gomes T, Mamdani MM, Gladstone DJ, Kapral MK (2011) The safety of proton pump inhibitors and clopidogrel in patients after stroke. Stroke 42(1):128–132
Liabeuf S, Lambert O, Metzger M, Hamroun A, Laville M, Laville SM, Chronic Kidney Disease-Renal Epidemiology and Information Network (CKD REIN) study group et al (2021) Adverse outcomes of proton pump inhibitors in patients with chronic kidney disease: the CKD-REIN cohort study. Br J Clin Pharmacol 87(7):2967–2976
Lo CH, Ni P, Yan Y, Ma W, Joshi AD, Nguyen LH et al (2022) Association of proton pump inhibitor use with all-cause and cause-specific mortality. Gastroenterology 163(4):852–61.e2
Maggio M, Corsonello A, Ceda GP, Cattabiani C, Lauretani F, Buttò V et al (2013) Proton pump inhibitors and risk of 1-year mortality and rehospitalization in older patients discharged from acute care hospitals. JAMA Intern Med 173(7):518–523
Mahabaleshwarkar RK, Yang Y, Datar MV, Bentley JP, Strum MW, Banahan BF et al (2013) Risk of adverse cardiovascular outcomes and all-cause mortality associated with concomitant use of clopidogrel and proton pump inhibitors in elderly patients. Curr Med Res Opin 29(4):315–323
Maret-Ouda J, Santoni G, Xie S, Rosengren A, Lagergren J (2022) Proton pump inhibitor and clopidogrel use after percutaneous coronary intervention and risk of major cardiovascular events. Cardiovasc Drugs Ther 36(6):1121–1128
Marker S, Krag M, Perner A, Wetterslev J, Lange T, Wise MP, SUP-ICU Trial Investigators et al (2019) Pantoprazole in ICU patients at risk for gastrointestinal bleeding-1-year mortality in the SUP-ICU trial. Acta Anaesthesiol Scand 63(9):1184–1190
Moayyedi P, Eikelboom JW, Bosch J, Connolly SJ, Dyal L, Shestakovska O, COMPASS Investigators et al (2019) Safety of proton pump inhibitors based on a large, multi-year, randomized trial of patients receiving rivaroxaban or aspirin. Gastroenterology 157(3):682-691.e2
Muñoz-Torrero JFS, Zamorano J, Rico-Martín S, Rivas MD, Bacaicoa MA, Robles R, FRENA Investigators et al (2020) Proton pump inhibitors and risk for recurrent ischemic events or death in outpatients with symptomatic artery disease. Atherosclerosis 292:84–89
Nayan M, Juurlink DN, Austin PC, Macdonald EM, Finelli A, Kulkarni GS, Canadian Drug Safety and Effectiveness Research Network (CDSERN) et al (2018) Medication use and kidney cancer survival: a population-based study. Int J Cancer 142(9):1776–1785
Oudit GY, Bakal JA, McAlister FA, Ezekowitz JA (2011) Use of oral proton pump inhibitors is not associated with harm in patients with chronic heart failure in an ambulatory setting. Eur J Heart Fail 13(11):1211–1215
Pani A, Pastori D, Senatore M, Romandini A, Colombo G, Agnelli F et al (2020) Clinical and pharmacological characteristics of elderly patients admitted for bleeding: impact on in-hospital mortality. Ann Med 52(7):413–422
Pegoli MA, Dedigama M, Mangoni AA, Russell PT, Grzeskowiak LE, Thynne T (2017) Proton pump inhibitors and risk of readmission and mortality in older patients discharged from a tertiary hospital to residential aged care facilities. Ther Adv Drug Saf 8(4):137–139
Rassen JA, Choudhry NK, Avorn J, Schneeweiss S (2009) Cardiovascular outcomes and mortality in patients using clopidogrel with proton pump inhibitors after percutaneous coronary intervention or acute coronary syndrome. Circulation 120(23):2322–2329
Roberts G, Pegoli M, Grzeskowiak L, Benger S, Forbes H, Hunt K et al (2021) Hospital admission as a deprescribing triage point for patients discharged to Residential Aged Care Facilities. Age Ageing 50(5):1600–1606
Rooney MR, Bell EJ, Alonso A, Pankow JS, Demmer RT, Rudser KD et al (2021) Proton pump inhibitor use, hypomagnesemia and risk of cardiovascular diseases: the Atherosclerosis Risk in Communities (ARIC) Study. J Clin Gastroenterol 55(8):677–683
Sturm L, Muller L, Schultheiss M, Binder B, Huber JP, Thimme R et al (2021) Proton pump inhibitor therapy is associated with reduced survival following first-time transarterial chemoembolization in patients with hepatocellular carcinoma. Eur J Gastroenterol Hepatol 33(1S Suppl 1):e247–e253
Teramura-Grönblad M, Bell JS, Pöysti MM, Strandberg TE, Laurila JV, Tilvis RS et al (2012) Risk of death associated with use of PPIs in three cohorts of institutionalized older people in Finland. J Am Med Dir Assoc 13(5):488.e9-e13
Tomisaki I, Harada M, Minato A, Nagata Y, Kimuro R, Higashijima K et al (2022) impact of the use of proton pump inhibitors on pembrolizumab effectiveness for advanced urothelial carcinoma. Anticancer Res 42(3):1629–1634
Tran T, Assayag D, Ernst P, Suissa S (2021) Effectiveness of proton pump inhibitors in idiopathic pulmonary fibrosis: a population-based cohort study. Chest 159(2):673–682
Tsai IJ, Lai TS, Shiao CC, Huang TM, Wang CH, Tsao CH et al (2020) Proton pump inhibitors augment the risk of major adverse cardiovascular events and end-stage renal disease in patients with acute kidney injury after temporary dialysis. Clin Pharmacol Ther 107(6):1434–1445
Wang X, Liu Q, Halfdanarson ÓÖ, Zoega H, Sadr-Azodi O, Engstrand L et al (2021) Proton pump inhibitors and survival in patients with colorectal cancer: a Swedish population-based cohort study. Br J Cancer 125(6):893–900
Wilson N, Gnjidic D, March L, Sambrook P, Hilmer SN (2011) Use of PPIs are not associated with mortality in institutionalized older people. Arch Intern Med 171(9):866
Wu H, Jing Q, Wang J, Guo X (2011) Pantoprazole for the prevention of gastrointestinal bleeding high-risk patients with acute coronary syndromes. J Crit Care 26(4):434.e1-e6
Xie J, Chen Q, He D (2022) Pre-existing proton pump inhibitor treatment and short-term prognosis of acute myocardial infarction patients. Front Cardiovasc Med 9:919716
Ben-Eltriki M, Green CJ, Maclure M, Musini V, Bassett KL, Wright JM (2020) Do proton pump inhibitors increase mortality? A systematic review and in-depth analysis of the evidence. Pharmacol Res Perspect 8(5):e00651
Yepuri G, Sukhovershin R, Nazari-Shafti TZ, Petrascheck M, Ghebre YT, Cooke JP (2016) Proton pump inhibitors accelerate endothelial senescence. Circ Res 118:e36-42
Kucuk HF, Akyol H, Kaptanoglu L, Kurt N, Barisik NO, Bingul S et al (2006) Effect of proton pump inhibitors on hepatic regeneration. Eur Surg Res 38(3):322–328
Araujo JA, Zhang M, Yin F (2012) Heme oxygenase-1, oxidation, inflammation, and atherosclerosis. Front Pharmacol 3:119
Shiraev TP, Bullen A (2018) Proton pump inhibitors and cardiovascular events: a systematic review. Heart Lung Circ 27(4):443–450
Song HJ, Rhew K, Lee YJ, Ha IH (2021) Acid-suppressive agents and survival outcomes in patients with cancer: a systematic review and meta-analysis. Int J Clin Oncol 3(1):34–50
Li T, Xie Y, Al-Aly Z (2018) The association of proton pump inhibitors and chronic kidney disease: cause or confounding? Curr Opin Nephrol Hypertens 27(3):182–187
Funding
This work was supported by the Postdoctoral Research Program of Sungkyunkwan University (2017).
Author information
Authors and Affiliations
Contributions
HJS was involved in study concept and design, literature search, data extraction, data analysis, data interpretation, and manuscript writing. HJS was involved in data interpretation and manuscript writing. XJ was involved in literature search, data extraction, and data interpretation. NJ, YJL, and IHH were involved in literature search and data interpretation. All authors reviewed and approved the final version.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interest
The authors declare no competing interests.
Additional information
Registration: The PROSPERO registration number is CRD42020179631.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• Little is known about the excess risk of death associated with proton pump inhibitor use in the elderly.
• We conducted a systematic review and meta-analysis of randomized controlled trials and observational studies regarding the association between proton pump inhibitors and the risk of death in adults aged 50 years or older.
• Our meta-analysis found a 15% increased risk of death in elderly people with PPI use compared to nonusers. Longer follow-up and cohort studies revealed an increased risk of death among older patients with cancers, cardiovascular disease, and kidney disease.
• Awareness of the increased mortality with PPI use should be raised, and the need to limit PPI prescriptions to the elderly where the benefits outweigh the potential risks should be emphasized.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, H.J., Seo, HJ., Jiang, X. et al. Proton pump inhibitors associated with an increased risk of mortality in elderly: a systematic review and meta-analysis. Eur J Clin Pharmacol 80, 367–382 (2024). https://doi.org/10.1007/s00228-023-03606-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-023-03606-0